Every minute a surgical patient spends in a cold operating room without proper thermoregulation is a minute of silent risk. A hospital patient warming suit is no longer a luxury add-on — it is a non-negotiable standard of care. Yet thousands of operating theatres across India, the USA, and Europe still rely on outdated gowns and blankets that leave patients dangerously exposed to anaesthesia-induced hypothermia.
This guide cuts through the noise. You will understand exactly what a hospital patient warming suit does, why perioperative hypothermia is deadlier than most surgical teams acknowledge, and how investing in the right forced air warming system for surgery can transform patient outcomes, reduce costs, and move your facility to the top of quality benchmarks.
What Is a Hospital Patient Warming Suit?
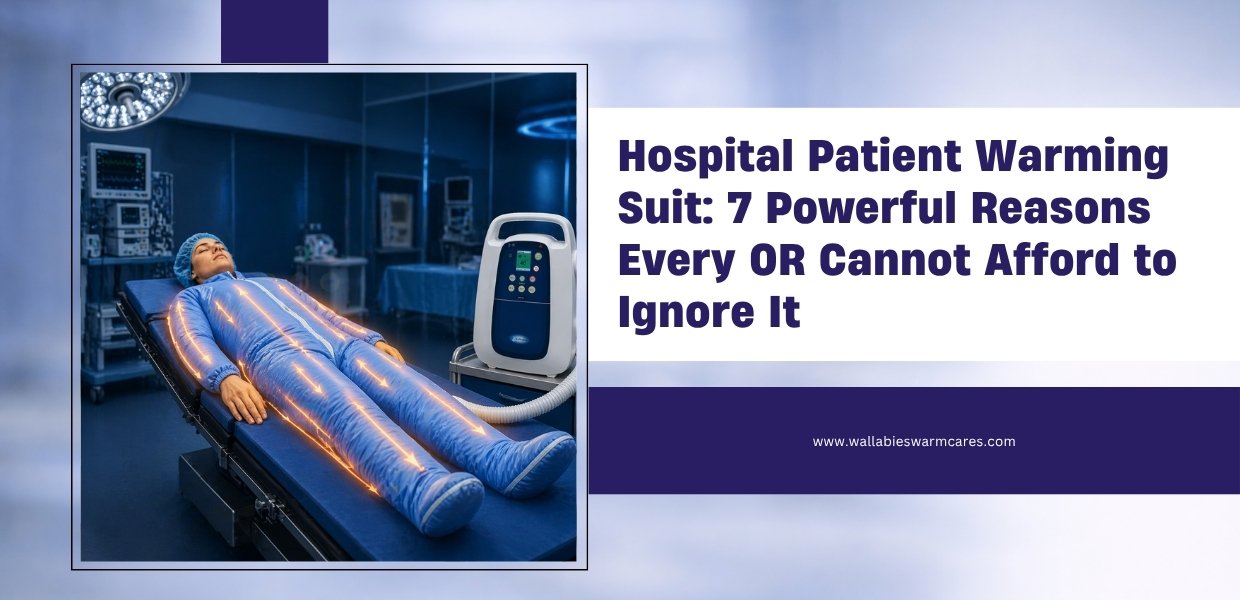
A hospital patient warming suit is a full-coverage, thermally engineered garment designed to maintain a patient’s core body temperature before, during, and after surgical procedures. Unlike a standard warming blanket draped over part of the body, a warming suit envelopes a larger surface area — arms, torso, and lower limbs — providing comprehensive, consistent heat delivery.
Modern warming suits are typically connected to a forced air warming (FAW) unit that pumps filtered, temperature-controlled air through micro-perforated channels within the suit fabric. This convective mechanism ensures uniform heat distribution, keeping patients in the clinically safe normothermia range of 36°C–37.5°C throughout the perioperative period. The key distinction between a suit and a standard blanket is coverage: suits reduce exposed skin surface area significantly, cutting radiative and convective heat loss at the source
The Hidden Crisis: Why Perioperative Hypothermia Prevention Matters More Than You Think
Inadvertent perioperative hypothermia — defined as a core body temperature below 36°C during or after surgery — affects a significant proportion of all surgical patients who are not actively warmed. Healthcare professionals increasingly recognise the hospital patient warming suit as the most comprehensive solution to this widespread problem. The consequences extend far beyond post-operative shivering.
Clinically documented complications include:
- Cardiac events — Cold-induced vasoconstriction raises afterload, increasing myocardial oxygen demand
- Surgical site infections (SSI) — Hypothermia impairs immune function and reduces tissue oxygen tension, creating ideal conditions for bacterial growth
- Coagulopathy — Enzyme activity in the clotting cascade drops significantly below normal temperature, increasing intraoperative blood loss
- Delayed wound healing — Reduced peripheral perfusion slows collagen synthesis
- Prolonged PACU stays — Patients who arrive hypothermic to recovery require active rewarming, extending bed occupancy and costs
- Increased anaesthesia drug requirements — Hypothermic patients metabolise drugs more slowly, demanding careful dosing adjustments
A landmark study published in PMC (2021) confirmed that combining active and passive warming systems is the most effective approach to prevent these complications, recommending pre-warming begin 20–30 minutes before anesthesia induction. A hospital patient warming suit used from the pre-operative ward is the most practical way to achieve this. Clinical evidence consistently shows that facilities that adopt a hospital patient warming suit protocol see measurable reductions in hypothermia-related complications.
7 Powerful Reasons to Upgrade to a Hospital Patient Warming Suit
1. Superior Full-Body Coverage for Consistent Patient Thermoregulation During Surgery
Standard warming blankets cover 40–60% of the body at best. A purpose-built hospital patient warming suit covers the upper body, midsection, and limbs simultaneously. This dramatically reduces the surface area through which heat escapes — the largest driver of intraoperative temperature loss.
Patient thermoregulation during surgery depends on minimising all four modes of heat loss: radiation, convection, conduction, and evaporation. Only a full-coverage suit addresses all four in a single intervention.
2. Forced Air Warming System for Surgery: Active + Passive in One Device
When a warming suit is paired with a quality forced air warming system for surgery, patients benefit from both active heat delivery (the FAW unit) and passive insulation (the suit fabric). Research shows this combined approach outperforms either intervention alone.
Wallabies Warm Care’s forced air warming system is engineered to work seamlessly with its warming suit range, delivering microprocessor-controlled, HEPA-filtered warm air at clinically optimal temperatures.
3. Reduced Surgical Site Infection Rates
Surgical site infections cost healthcare systems billions annually and can extend a patient’s hospital stay by a week or more. Maintaining normothermia through proper use of a hospital patient warming suit has been clinically linked to measurable reductions in SSI rates. For hospitals under pressure on quality metrics — particularly in India’s NABH accreditation framework, the USA’s Joint Commission standards, and European CE-marked device regulations — this outcome matters enormously.
4. Shorter Hospital Stays and Lower Costs Per Patient
Every extra PACU hour or ICU day carries real financial and operational costs. When perioperative hypothermia prevention is achieved through a pre-to-post warming protocol using a hospital patient warming suit, patients recover faster, consume fewer rewarming resources, and are discharged sooner. Across both public and private hospitals, the return on investment from implementing a standardised hospital patient warming suit programme is consistently positive. The economics are compelling for hospital procurement committees in any geography.
5. Improved Patient Comfort and Satisfaction Scores
Patients remember how they felt before surgery. A patient who enters the OR warmly wrapped in a thermal suit reports lower pre-operative anxiety and greater satisfaction, even before the clinical benefits are considered. As HCAHPS scores in the USA and NHS patient satisfaction surveys in Europe increasingly influence hospital reimbursements and ratings, this soft benefit has hard financial value.
6. Adaptable to All Surgery Types and Patient Profiles
Modern warming suits are designed with surgical access points and openings for IV lines, catheter access, and anaesthesia monitoring that do not compromise coverage. Paediatric, adult, and bariatric configurations are available. Whether the case is a 30-minute outpatient procedure or a 6-hour open abdominal surgery, there is a hospital patient warming suit configuration to match.
7. Regulatory Compliance Across India, USA, and Europe
Hospitals in India operating under NMC guidelines, US facilities under CMS and Joint Commission oversight, and European hospitals complying with EU MDR 2017/745 all face growing pressure to document active temperature management. A structured warming protocol built around a hospital patient warming suit and connected FAW unit provides a clear, auditable clinical pathway.
How a Forced Air Warming Suit Works: A Step-by-Step Protocol

A best-practice perioperative warming protocol using a hospital patient warming suit follows four stages. Selecting the right hospital patient warming suit for your OR is the first critical decision in this process:
Stage 1 — Pre-operative (30 min before induction): The patient is fitted with the warming suit in the pre-op ward. The FAW unit begins at a preset temperature, pre-warming the patient’s thermal periphery and reducing the redistribution drop that occurs at anaesthesia induction.
Stage 2 — Intraoperative: The suit remains in place throughout surgery. The FAW unit is adjusted per the anaesthesiologist’s protocol. Core temperature is monitored continuously using an esophageal, nasopharyngeal, or zero-heat-flux sensor.
Stage 3 — Post-operative / PACU: If core temperature is confirmed at 36°C or above, the FAW unit is weaned. The insulating hospital patient warming suit maintains warmth passively during the transition, preventing post-operative temperature drop.
Stage 4 — Ward Transfer: For longer recoveries, a lightweight passive insulation suit continues thermal protection until the patient is fully stable.
Surgical Warming Blanket for Hospitals vs. Patient Warming Suit: Which Should You Choose?
A surgical warming blanket for hospitals remains useful in specific contexts — underbody warming during long prone cases, upper-body coverage during lower-limb procedures, and neonatal/paediatric applications where a full suit may be impractical.
However, for the majority of adult surgical patients, a hospital patient warming suit offers superior thermoregulatory outcomes because of its full-body design. The clinical literature increasingly supports a suit-first approach for at-risk patients: elderly, diabetic, patients on thyroid or psychotropic medications, and any procedure exceeding 60 minutes under general anaesthesia.
The most effective hospital warming programmes use both a hospital patient warming suit for the perioperative period, with targeted blankets for specific positional or access requirements intraoperatively.
Why Wallabies Warm Care Is the Right Partner
Wallabies Warm Care is a leading producer and supplier of forced air warming systems and hospital patient warming suit solutions designed to the highest medical standards. Our microprocessor-controlled warming units and micro-perforated warming blankets are engineered for hospitals, operation theatres, and intensive care units across India, North America, and Europe.
We understand that procurement decisions in healthcare are driven by clinical evidence, cost-efficiency, and compliance. Our hospital patient warming suit range addresses all three — combining proven FAW technology with suit designs that adapt to your surgical workflow without disruption.
For the latest clinical guidelines on perioperative temperature management, refer to the WHO Surgical Safety Checklist guidelines: WHO Safe Surgery Guidelines
➜ Explore our full patient warming system range here
Frequently Asked Questions (FAQ)
Q: What is a hospital patient warming suit used for?
A: A hospital patient warming suit is used to maintain a surgical patient’s core body temperature before, during, and after procedures, preventing inadvertent perioperative hypothermia and its associated complications.
Q: Is a patient warming suit better than a warming blanket?
A: For full-body thermoregulation, a warming suit covers more surface area and provides superior results. Warming blankets are better for targeted or positional applications. Many hospitals use both.
Q: How does a forced air warming system work with a warming suit?
A: The FAW unit pumps clean, temperature-regulated air through channels in the suit fabric, delivering uniform convective heat across the patient’s body.
Q: What temperature should a warming suit be set at?
A: This depends on the clinical protocol, but most guidelines recommend maintaining core temperature above 36°C. Pre-warming at 38–40°C for 20–30 minutes before induction is widely recommended.
Q: Are patient warming suits compliant with Indian hospital standards?
A: Yes. A quality hospital patient warming suit meeting ISO 13485 and relevant IEC 60601 standards is appropriate for use in NABH-accredited facilities across India.